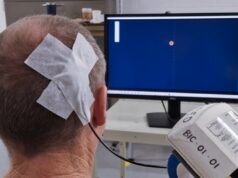
 By delivering small electrical pulses directly to the brain, deep brain stimulation (DBS) can ease tremors associated with Parkinson’s disease or help relieve chronic pain. The technique works well for many patients, but researchers would like to make “next-generation” DBS devices that are a little smarter by adding the capability to sense activity in the brain and adapt stimulation accordingly—and a new algorithm developed by Brown University bioengineers could enable progress on this front by removing a key hurdle that makes it difficult for DBS systems to sense brain signals while simultaneously delivering stimulation.
By delivering small electrical pulses directly to the brain, deep brain stimulation (DBS) can ease tremors associated with Parkinson’s disease or help relieve chronic pain. The technique works well for many patients, but researchers would like to make “next-generation” DBS devices that are a little smarter by adding the capability to sense activity in the brain and adapt stimulation accordingly—and a new algorithm developed by Brown University bioengineers could enable progress on this front by removing a key hurdle that makes it difficult for DBS systems to sense brain signals while simultaneously delivering stimulation.
“We know that there are electrical signals in the brain associated with disease states, and we would like to be able to record those signals and use them to adjust neuromodulation therapy automatically,” said David Borton, an assistant professor of biomedical engineering at Brown University in Providence, USA and corresponding author of the study describing the algorithm. “The problem is that stimulation creates electrical artifacts that corrupt the signals we are trying to record. So, we have developed a means of identifying and removing those artifacts, so all that is left is the signal of interest from the brain.”
The research, which is published in the open access journal Cell Reports Methods, was co-led by Nicole Provenza, a PhD candidate working in Borton’s lab at Brown University, and Evan Dastin-van Rijn, a PhD student at the University of Minnesota who also worked on the project while he was an undergraduate at Brown University. Borton’s lab is affiliated with Brown University’s Carney Institute for Brain Science.
There are several factors that make it difficult to sense and stimulate via an implantable DBS system at the same time, the researchers note in their report. For one thing, the frequency signature of the stimulation artifact can sometimes overlap with that of the brain signal researchers want to detect, meaning that merely cutting out swaths of frequency to eliminate artifacts might also remove important signals. To eliminate the artifact and leave other data intact, the exact waveform of the artifact needs to be identified, which presents another problem. Implanted brain sensors are generally designed to run on minimal power, so the rate at which sensors sample electrical signals makes for fairly low-resolution data, and accurately identifying the artifact waveform with such low-resolution data is a challenge.
To get around that problem, the Brown University researchers came up with a way to turn low-resolution data into a high-resolution picture of the waveform. Even though sensors do not collect high-resolution data, they do collect a large amount of data over time. According to a Brown University press release, the team found a way to cobble bits of data together into a high-resolution picture of the artifact waveform using mathematics.
“We basically take an average of samples recorded at similar points along the artifact waveform,” Dastin-van Rijn said. “That allows us to predict the contribution of the artifact in those kinds of samples, and then remove it.”
In a series of laboratory experiments and computer simulations, the team showed that their algorithm outperforms other techniques in its ability to separate signal from artifact. The team also used the algorithm on previously collected data from humans and animal models to show that they could accurately identify artifacts and remove them.
“I think one big advantage to our method is that even when the signal of interest closely resembles the simulation artifact, our method can still tell the difference between the two,” Provenza said. “So, that way, we are able to get rid of the artifact while leaving the signal intact.”
Another advantage, the researchers say, is that the algorithm is not computationally expensive. It could potentially run in real time on current DBS devices, they add, opening the door to real-time artifact-filtering, which would enable simultaneous recording and stimulation.
“That is the key to an adaptive system,” Borton stated. “Being able to get rid of the stimulation artifact while still recording important biomarkers is what will ultimately enable a closed-loop therapeutic system.”