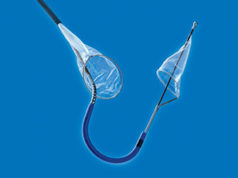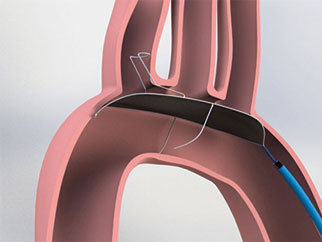
Plans to initiate clinical trials for a new, advanced version of the TriGuard cerebral embolic protection device (Keystone Heart) have been announced.
According to the company, this third-generation device, TriGuard 3, will continue the TriGuard legacy of being the only device designed to provide full coverage of all cerebral vessels while protecting the brain from embolic debris resulting from heart procedures, and also offer technological improvements over earlier versions of the device. Keystone Heart has accelerated the development programme to enable initiation of third-generation device trials by the end of the year.
Like earlier TriGuard devices, TriGuard 3 is designed to protect the brain from emboli during transcatheter aortic valve implantation (TAVI) and other heart procedures to minimise the risk of stroke and other potential damage to the brain. Unique to its design, TriGuard 3 is focused on ease of use, and an ability to minimise interactions with other heart procedure devices. The new device is designed for universal patient application by being anatomy independent and does not interact with any of the cerebral branch vessels. TriGuard 3 incorporates an over the wire design via an 8F sheath.
“We need the right tools to best combat the risk of stroke and neurological damage associated with TAVI and other cardiovascular procedures. We know that embolic debris resulting from these procedures can have a grave impact on how post-procedure patients function in their daily lives. Having personally been involved in TriGuard 3 testing, the new improvements to TriGuard enhance its ability to become the optimal design for cerebral embolic protection,” said Jeffrey Moses, professor of Medicine at Columbia University College of Physicians and Surgeons, director of Interventional Cardiac Therapeutics at New York-Presbyterian Hospital/Columbia University Medical Center, and director of Advanced Cardiac Therapeutics at St Francis Heart Center, New York, USA.
The number of TAVI procedures conducted in the USA each year has increased exponentially in the past six years, with more than 24,000 conducted in 2015 according to a report issued in March 2017. About 94% of patients have new brain lesions after TAVI, one out of four have some neurological impairment after TAVI, and four out of 10 have some neurocognitive worsening one month after TAVI. Moderate to mild brain injuries, which are caused by new lesions in the brain, can affect the patient’s processing speed, executive function, and fundamental skills such as memory, language, and balance. These lesions may be related to changes in the way your brain functions or processes information, and lesions in the brain stem can impact basic body functions such as breathing, swallowing, heart rate, blood pressure, consciousness, and whether one is awake or fatigued.
Previously released data demonstrate significantly reduced stroke rates, as well as significantly reduced total lesion volume for patients with complete coverage of all cerebral branches using the second-generation TriGuard device compared to those who were unprotected. These data are based on a pooled analysis of three trials with a total of 142 patients undergoing TAVI with TriGuard.
All patients enrolled in the current REFLECT study, a multicentre, phase 2/3, randomised, interventional, single-blind clinical study designed to evaluate the safety and efficacy of the second-generation TriGuard embolic deflection device, will continue to be evaluated post-procedure, and results will remain blinded. The trial will not enrol any additional patients in order to initiate the TRIFLECT study, which will evaluate TriGuard 3.