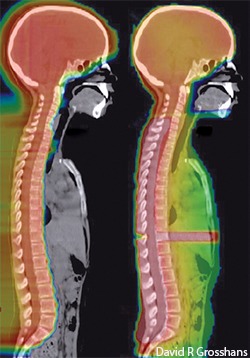
 A study has shown that the treatment of medulloblastoma with proton beam therapy may be as safe as conventional photon-based radiotherapy. The treatment was shown to have similar survival rates to conventional radiotherapy in the study led by Torunn Yock, Massachusetts General Hospital, Proton Center, Boston, USA, and colleagues, published in The Lancet Oncology.
A study has shown that the treatment of medulloblastoma with proton beam therapy may be as safe as conventional photon-based radiotherapy. The treatment was shown to have similar survival rates to conventional radiotherapy in the study led by Torunn Yock, Massachusetts General Hospital, Proton Center, Boston, USA, and colleagues, published in The Lancet Oncology.
In this new study, funded by the US National Cancer Institute and Massachusetts General Hospital, a total of 59 patients aged from three to 21 years were enrolled between 2003 and 2009. Most patients (55) had the tumour partially or completely removed through surgery. All patients (59) received chemotherapy as well as proton beam therapy. On average, patients were followed-up for seven years.
At three years after treatment, 12% of patients had serious hearing loss. This rose to 16% at five years. Patients also displayed problems with processing speed and verbal comprehension, but perceptual reasoning and working memory were not significantly affected. At five years, over half (55%) had problems with the neuroendocrine system which regulates hormones – with growth hormone being the most commonly affected. However, the study reported no cardiac, pulmonary, or gastrointestinal toxic effects which are common in patients treated with photon radiotherapy.
At three years after treatment, progression-free survival was 83%. At five years, progression-free survival was 80%.
The authors say, “Our findings suggest that proton radiotherapy seems to result in an acceptable degree of toxicity and had similar survival outcomes to those achieved with photon-based radiotherapy. Although there remain some effects of treatment on hearing, endocrine, and neurocognitive outcomes—particularly in younger patients—other late effects common in photon-treated patients, such as cardiac, pulmonary, and gastrointestinal toxic effects, were absent.”
They conclude, “Proton radiotherapy resulted in acceptable toxicity and had similar survival outcomes to those noted with conventional radiotherapy, suggesting that the use of the treatment may be an alternative to photon-based treatments.”
Writing in a linked comment, David R Grosshans, Department of Radiation Oncology, University of Texas MD Anderson Cancer Center, Houston, USA, says, “I believe that radiation oncologists have always understood that our treatments are associated with the potential for severe adverse effects. I also believe that many in radiation oncology embrace new technology, not simply to have the latest and greatest innovations, but rather to reduce the effect of radiation therapy on patients’ quality of life. Nowhere in oncology is this more important than for paediatric cancers.”
He concludes, “This study sets a new benchmark for the treatment of paediatric medulloblastoma and alludes to the clinical benefits of advanced radiation therapies.”
Two UK centres for proton beam therapy (in Manchester and London) are currently being planned which are due to open in 2018.