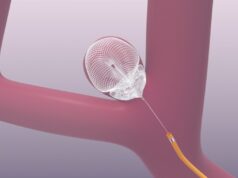
Covidien has announced that the final results of the PUFs (Pipeline for uncoilable or failed aneurysms) clinical study of its Pipeline embolization device have been published in the June issue of Radiology.
The Pipeline device, according to a press release, met the trial’s primary endpoints for both effectiveness and safety. Based on these data, the Pipeline device was approved by the US Food and Drug Administration (FDA) on 6 April 2011.
“Patients with an unruptured large or giant wide-necked aneurysm in the internal carotid artery are at significant risk of death or a highly disabling stroke and other significant neurologic complications if the aneurysm bursts or pushes on surrounding nervous tissues,” said principal investigator Tibor Becske, assistant professor, Departments of Radiology, Division of Neuro Interventional Radiology and Neurology at NYU Langone Medical Center in New York, USA. “This study of highly complex aneurysms confirms that, for certain patients, there is a safe and effective minimally-invasive procedure to address the underlying pathology of the aneurysm— allowing the vessel to heal over time.”
“The Pipeline device offers hope for those patients who have had poor alternatives for treating this often debilitating and sometimes fatal medical condition,” said Christine Buckley, executive director of the Brain Aneurysm Foundation.
Traditional endovascular methods of treating these aneurysms have included a reconstructive approach of filling the aneurysm sac with an embolic material (usually detachable coils), or parent artery occlusion, where doctors attempt to close off the affected artery. However, neither of these approaches addresses the underlying pathology of the aneurysm.
Overall, 108 patients were enrolled into the study. Of the 106 evaluable aneurysms that were treated with one or more Pipeline devices, 73.6% completely closed (p-value <.0001) without the use of an alternative treatment. Importantly, the occlusion rate in these patients also improved over time, reaching 86.8% complete occlusion at one-year follow-up. These occlusion rates are significant, especially for this challenging patient population.
Investigators compared the Pipeline device to historical controls because no other blood flow diverting devices are available in the USA. Effectiveness of stents has not been proven to FDA standards; and outcomes for surgical or other endovascular treatments have been suboptimal.
Investigators measured safety of the device by the number of patients who suffered an ipsilateral stroke or neurologic death in the 180 days following the procedure. In the study, six of 107 (5.6%) patients (p-value <.0001) suffered one of these events, significantly less than the predefined safety threshold of 20%. The 20% threshold was based on a literature review of adverse events rates associated with other current procedures and therapies.
“Covidien remains committed to delivering clinical data to help redefine how neurointerventionalists treat large and giant wide-necked aneurysms,” said Mark A Turco, Chief Medical Officer, Vascular Therapies, Covidien. “The publication of the PUFs pivotal data represents an important milestone for the company and we look forward to continuing to work with the medical community to deliver additional evidence to support new treatment options for patients.”