This advertorial is sponsored by Perflow.
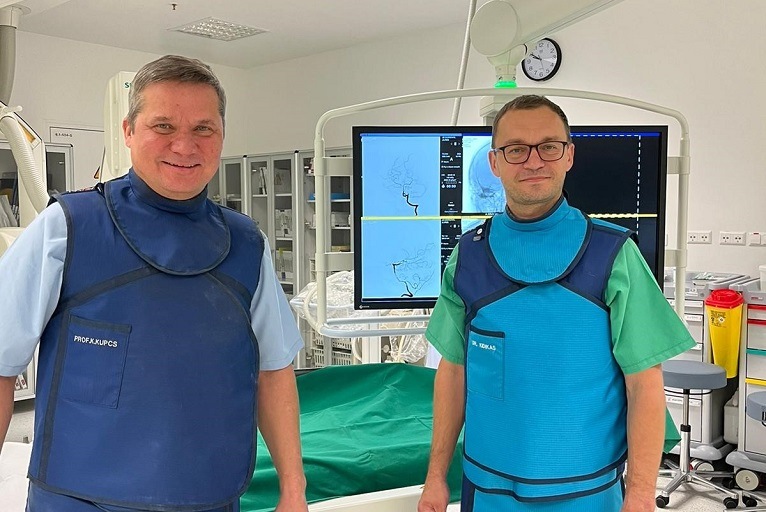
The StreamTM family of products (Perflow) is a range of dynamic neurothrombectomy net devices designed to give physicians greater control and visibility when treating ischaemic stroke. The first clinical use of the Stream17—a lower-profile device intended to improve the treatment of more tortuous patient anatomies—was announced in May 2021, with preliminary data on Stream technology as a whole being presented even more recently at the Barts Research and Advanced Interventional Neuroradiology conference (BRAIN 2021; 13–16 December, London, UK). Kārlis Kupčs and Helmuts Kidikas of the Pauls Stradiņš Clinical University Hospital (Riga, Latvia) discuss their experiences with Stream, and the data their centre has collected on this next-generation stent retriever.
A
Could you briefly outline your experience with the Stream device to date?
We performed our first endovascular thrombectomy procedure back in 2006—which was also the first time this procedure had ever been done in Latvia—and, over the course of the past 15 years, we have had the opportunity to use pretty much all of the thrombectomy devices that are on the market. And, in that time, we have gained a lot of experience with these devices, performing close to 1,500 cases.
We started with the Stream devices in 2019, and we were one of the first centres that had the opportunity to use this technology. Up to now, we have deployed them in more than 40 cases. The majority of these cases have been with the standard device—which has undergone several improvements since 2019. More recently, we have also had the chance to use the Stream XL, which we use for large vessel occlusions (LVOs), and Stream17, which is one of the more unique devices on the market right now.
What are the most appropriate cases and anatomies to use this technology in?
As you would expect, we use the standard Stream devices for standard cases! Specifically, M1 occlusions and also basilar artery occlusions are instances in which the standard Stream performs very well. We have also found that certain, more complex cases, such as when the thrombus is very hard and cartilage-like, are easier to handle with the Stream compared to other stent retrievers because you can manually adjust the device and thus the radial force applied to the arterial wall.
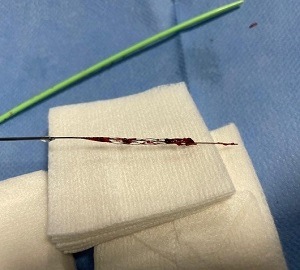
The Stream17 device is one of the smallest thrombectomy devices on the market and, as such, it can be deployed via microcatheters with an inner diameter as small as 0.017 inches, meaning you can navigate to more distal anatomies like M2 or M3 branches, and perform thrombectomies there. And, of course, the advantage of using these smaller microcatheters is that it makes your distal catheterisation quicker and easier. We have done a couple of cases involving posterior cerebral artery occlusions too, specifically in the P1 and P2 segments, and the Stream17 worked very nicely.
Overall, there are probably not any cases that you could look at and say: “This is not a Stream case”. You can use Stream for any case—it is just about choosing the right size between the standard device, the Stream XL and the Stream17.
What features do you appreciate the most on the Stream device?
The Stream is a very special device, because it is one of the only dynamic thrombectomy devices on the market. Whereas many other stent retrievers are self-expanding—meaning you have no control over how far the stent retriever expands—the Stream gives you full control over how far, and with how much force, the braid will open. This is especially important in more difficult cases, as that extra control means we can make adjustments in real-time, helping us to remove the thrombus more safely and sometimes more quickly, which, of course, brings benefits for the patient.
Another great feature of the Stream is its radiopacity. Under fluoroscopic guidance, the device is fully radiopaque and can be visualised on imaging software once it has been deployed and opened—which is not the case for most stent retrievers. This visibility helps to give you a better idea of how the device is interacting with the thrombus, and also where the thrombus is positioned relative to the device during clot retrieval. The device’s excellent visibility combined with how controllable it is allows us, as treating physicians, to apply our knowledge and experience directly and precisely at the occlusion site within the vessel.
Is it easy to use the Stream?
As with any stent retriever, there is obviously a learning curve regarding how to handle the specific device and how best to use all of its functionalities. One needs to familiarise themself with the device’s dimensions, its length and the radiopaque markers. You also need to get used to the different settings—auto-lock mode and free mode—that the handle enables. One of our suggestions would be to take care not to over-expand the device unnecessarily, as we found this can happen when we first started using Stream. As a starting point, you can use four or five ‘clicks’ to open the device in auto-lock mode and, in our experience, it will still function perfectly well without needing to be fully expanded.
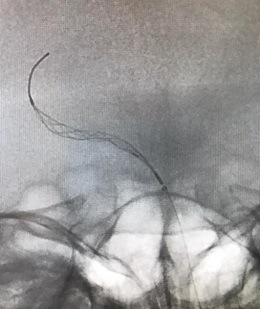
Overall, you probably need to perform about 10 cases to become completely familiar with the handling of the device. But, from then on, it will enable you to have more precise control during thrombectomy procedures. The difference between the Stream and a self-expanding stent retriever is like the difference between driving a car with a manual gearbox or an automatic transmission. With the Stream, you need to choose what gear you are in, but once you have mastered that skill it opens up more possibilities and enables you to offer the patient a better chance of reaching the limits of what can be achieved—with the goal of removing the thrombus quickly and effectively.
Have you seen any complications while using the device?
When you are treating ischaemic stroke, it is impossible to have no complications at all. However, in our data, the rates of device-related and/or overall complications are no higher than those seen with other stent retrievers.
Could you highlight some key findings from the data you have collected on the Stream to date?
It is important to note that we are still in the process of collecting and analysing these data. However, in terms of recanalisation rates—which we often look at when it comes to device performance—the numbers are really high compared to other thrombectomy devices.
At the recent BRAIN conference, we presented data demonstrating successful recanalisation (Class 3 or 2b, thrombolysis in cerebral infarction [TICI] scale) in about 90% of patients treated between February and December 2021 (n=41, 51% male, mean age=70 years). These patients had a mean preprocedure National Institutes of Health Stroke Scale (NIHSS) score of 16 and we observed an average procedure duration of 54 minutes.
These data are only from a single centre, however, and as such we believe that a multicentre study would now be a very good option to expand the existing body of data on Stream, and its performance as an acute ischaemic stroke treatment.
Kārlis Kupčs is the head of the Diagnostic Radiology Institute, and an assistant professor and interventional radiologist, at the Pauls Stradiņš Clinical University Hospital in Riga, Latvia.
Helmuts Kidikas is an interventional radiologist in the Diagnostic Radiology Institute at the Pauls Stradiņš Clinical University Hospital in Riga, Latvia.
DISCLAIMER: The Stream device has received CE certification for use in Europe but is currently not available for sale in the USA.













