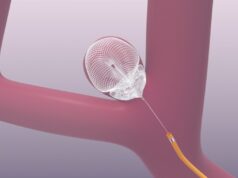
Alejandro M Spiotta, Department of Neurosurgery, Medical University South Carolina, Charleston, USA, reported his team’s experience with the new balloon-stent technique for intracranial aneurysm treatment using the Scepter C balloon catheter and the LVIS, a low-profile visualised intraluminal stent.
The first use of the novel balloon-stent technique for the treatment of intracranial aneurysms has been revealed in a paper led by Alejandro M Spiotta, Department of Neurosugery, Medical University South Carolina, Charleston, USA, published ahead-of-print in the Journal of Neurointerventional Surgery. The authors explained that the balloon-stent method proposed in this paper involves stent placement after completition of a balloon assisted coil embolization. The authors used the Scepter C (MicroVention) balloon in conjunction with a low-profile visualised intraluminal stent, the LVIS 2.5mm x 16mm stent (MicroVention).
“The introduction of balloon remodelling and stent-assisted coil embolization are two advances which have revolutionised the treatment of wide-necked aneurysms,” the authors explained. According to the literature, the authors reported, “Balloon remodelling involves the temporary inflation of a balloon across the neck of an aneurysm allowing for coil deployment into aneurysms with unfavourable neck to dome ratios. The technique of stent assisted coiling has also been widely adopted as a promising adjunct with potential mechanical, haemodynamic and biologic properties, imparting an advantage over coil embolization alone.” These two techniques may be used in combination to capitalise on the benefits provided by both, they commented.
The patient was a 51-year-old man with an unruptured middle cerebral artery bifurcation aneurysm which was treated with the balloon and, post coil embolization, the LVIS was delivered via the coaxial balloon catheter and deployed across the aneurysm neck. According to the results and follow-up angiograms the coil mass proved to be well-seated in the aneurysm sac and the parent vessel was patent.
The authors described the technique as follows: “Utilising an 18G Cook needle in a 6F Pinnacle sheath was placed into the right common femoral artery. Five thousand units of intravenous heparin and intermitted blouses were administered to maintain ACT 2—2.5 times the patient’s baseline. A 6F Neuro 070 guide catheter (Penumbra) with a 5F Berenstein diagnostic insert (Penumbra) was advanced into the aortic arch over a 0.038 inch Terumo Glidewire (MicroVention) to select the distal petrous segment of the internal carotid artery. Eight milligrams of verapamil was injected intra-arterially. Under roadmap guidance, a 4×4 Scepter C balloon catheter was advanced over a 0.014 inch Transcend EX platinum guidewire (Boston Scientific) into the inferior division branch and centred across the aneurysm neck.”
“An SL 10 microcatheter (Boston Scientific) was advanced over a 0.014 inch Trancent EX platinum guidewire into the middle cerebral aerty aneurysm. With intermittent balloon inflations lasting less than five minutes, the following Stryker (Boston Scientific) coils were introduced into the aneurysm and deployed. The microcatheter was removed. With the Scepter C balloon catheter kept in place, a LVIS 2.5mmx16mm stent was introduced centred across the aneurysm neck with the distal markers in the proximal M2 segment and the proximal markers in the mid M1 segment and the balloon catheter was withdrawn to unsheath and deploy the stent across the aneurysm neck and middle cerebral artery bifurcation.”
Spoitta et al said that the balloon-stent method does carry risk factors as it involves placement of the stent post balloon-assisted embolization which requires additional manoeuvres increasing the risk of coil disruption.
“In the case described, we found this technique to be safe and feasible, reducing both the number of steps involved in this technique and the opportunities for mechanical coil-related complications” concluded the authors. “We anticipate the adoption of this technique to be a valuable tool in the armamentarium of the neurointerventionalist.”