Doctors are relying increasingly on their hand-held communication devices to stay abreast of developments taking place in hospital when they are away. New research is suggesting that these devices could have an impact on stroke management.
A study published in the January 2012 issue of Stroke reports that researchers in Japan have developed a system involving the use of handheld communication devices for rapidly exchanging diagnostic images and clinical and management information.
Hiroyuki Takao, Department of Neurosurgery, Jikei University School of Medicine, Tokyo, Japan, and colleagues wrote in the paper that the role of telemedicine and timely coordination of the efforts of the stroke team have become important due to the increasing demand for rapid diagnosis and treatment of stroke.
Takao and colleagues created a system to communicate patient data and images between hospital systems, and participating staff members who were in and out of the hospital through their handheld communication devices. They devised the system so that it can transfer clinical data, CT, MR, angiographic, intraoperative images, and expert opinion in real time.
After a pilot application of the system in the hospital which showed successful information transfer, allowing medical staff to discuss patients’ diagnosis and management using a Twitter direct messaging system, the researchers concluded that the system (called i-Stroke) may become a useful tool for acute patient management in the field of neurology and neurosurgery.
Smartphone diagnosis of stroke
In 2011, a retrospective study from the University of Calgary, Canada, published in the Journal of Medical Internet Research on 6 May, suggested that physicians can make a stroke diagnosis using a smart phone application with the same accuracy as one made using a medical computer workstation. The study revealed that a new smartphone client-server teleradiology system appeared promising and had “the potential to allow urgent management decisions in acute stroke”.
Authors Ross Mitchell et al wrote that advances in the treatment of acute ischaemic stroke had made rapid acquisition, visualisation, and interpretation of images, a key factor for positive patient outcomes.
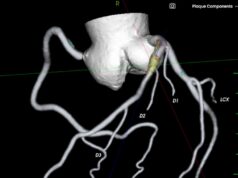
They then developed a new teleradiology system that enabled rapid access to interactive advanced 2D and 3D visualisation on a current generation smartphone device (Apple iPhone or iPod Touch, or an Android phone) without requiring patient image data to be stored on the device. Instead, a server loads and renders the patient images, then transmits a rendered frame to the remote device.
The researchers set out to determine whether the smartphone client-server teleradiology system was capable of providing accuracies and interpretation times sufficient for diagnosis of acute stroke.
Neuroradiologists in the study looked at 120 recent consecutive non-contrast computed tomography (NCCT) brain scans and 70 computed tomography angiogram (CTA) head scans that were obtained from the Calgary Stroke Program database.
The scans were read by two neuroradiologists, one on a medical diagnostic workstation and on an iPod touch or iPhone (both referred to as iOS device), and the other, only on an iOS device.
The results showed that there was a 94% to 100% rate of accuracy on the iOS device for diagnosing acute stroke compared with a medical workstation that has a much bigger screen.
The authors cautioned that this study was retrospective, involved relatively few patient studies, and only two readers. “Generalising conclusions about its clinical utility, especially in other diagnostic use cases, should not be made until additional studies are performed,” they wrote.
The technology discussed in the paper was transferred to a company co-founded by Mitchell, Calgary Scientific. The company used the technology to create the product ResolutionMD Mobile, which in September 2011 received clearance from the FDA for primary diagnostic use with MR and CT scans.
Bart M Demaerschalk, professor of Neurology and director, Cerebrovascular Diseases Center and Teleneurology and Telestroke Program, Department of Neurology, Mayo Clinic, told NeuroNews, “We incorporated ResolutionMD smartphone teleradiology application into the Mayo Clinic Telestroke Network in Arizona. Mayo Clinic smartphone teleradiology research study assessed the level of brain CT scan interpretation agreement between Mayo Clinic vascular neurologists (with ResolutionMD) and spoke hospital radiologists (standard PACS) against a reference standard. The results demonstrated that Mayo Clinic vascular neurologists preferred to view the CT of the acute stroke patient on ResolutionMD, compared with standard desk top or lap top DICOM viewers, in 80% of the telemedicine consultations. The ResolutionMD images were accessed an average of 11 minutes faster into the consults, and there was nearly perfect agreement with radiologists and reference standard. We concluded that ResolutionMD smartphone teleradiology can successfully be incorporated into telestroke network operations. The technical failure rate was very low. In only one of sixty-five consecutive subjects was transmission and retrieval of images to ResolutionMD problematic. We are now conducting a research study comparing remote neurological evaluation of acute stroke patients via live smartphone audio video face time function to standard face-to-face neurological examination—in order to understand its reliability and validity. We believe that mobile technology is beneficial for the assessment, diagnosis, and treatment of acute stroke patients in remote and rural communities where there may be no direct or timely access to neurological expertise.”
Since publication of the original paper Ross Mitchell has relocated to the Mayo Clinic in Scottsdale, Arizona, USA.