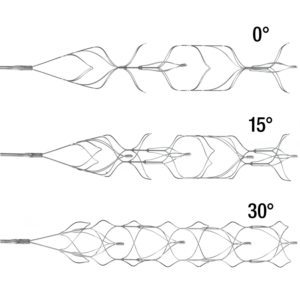
According to one presentation given at the Society of NeuroInterventional Surgery’s 14th Annual Meeting (SNIS; 24–27 July, Colorado Springs, USA) the 3D revascularisation device is a safe and effective device for mechanical thrombectomy and is a valuable adjunct to the ADAPT technique when aspiration alone fails to achieve mechanical recanalisation.
Josser Delgado (Abbott Northwestern Hospital, Minneapolis, USA) reported his centre’s experience with the 3D device. He explained that the 3D revascularisation device is designed to have less metal in contact with the vessel wall and more metal in contact with the clot. It has four intraluminal chambers and it is designed to be used in combination with a reperfusion catheter.
The 3D device is 26mm in length with a width of 4.5mm and has four radiopaque markers which correspond with each point of the different chambers. It has been designed and tested to be used for up to five retrieval passes and it can be delivered through a microcatheter.
Completed in 2016, the 3D trial was a multicentre randomised controlled trial comparing two thrombectomy techniques—the 3D revascularisation device plus aspiration versus aspiration only. The study included patients who had contraindications for IV t-PA and patients who were up to eight hours from time of last-known-well. Patients were enrolled between 29 May 2012 and 29 November 2017 at 25 centres in the USA. A total of 173 patients were included in the study, and of those, 87 were randomised to the 3D device plus aspiration arm and 86 were randomised to the aspiration only arm.
Delgado reported that there were no significant differences in the baseline characteristics of the patients, and there was a trend towards more ICA terminus clots in the aspiration only arm of the trial, puncture to reperfusion time was significantly shorter in the aspiration only arm compared to the 3D device plus aspiration arm. There was no statistically significant difference in the TICI 2b–3 rate between the two arms, and there was also no difference in the good outcome rate at 90 days (42% for 3D device plus aspiration vs. 48% for aspiration only).
Comparing the results with the 3D device with those from the HERMES meta-analysis, Delgado said that they were similar—TICI 2b–3: HERMES=71% vs. 3D RCT=79% vs. 3D device plus aspiration arm=84%.
Following the 3D trial, the device was approved for use in the USA and is now commercially available.
Finally, Delgado gave some tips for the best use of the 3D revascularisation device: “It is really designed to be used in combination with the ACE aspiration catheter. Also, you want to make sure that all four of the device markers are outside of the catheter for proper deployment of the device. It is safe to remove the microcatheter completely after the deployment of the 3D device—we do that so we can maximise the aspiration power of the ACE catheter as we are removing the 3D. Additionally, we try to advance the ACE catheter as close to the thrombus as possible while we are retrieving the 3D device, and then after we have removed the 3D we perform the ADAPT technique.”
He concluded, “the 3D device is a safe and effective device for mechanical thrombectomy and is a valuable adjunct to the ADAPT technique when aspiration alone fails to achieve mechanical recanalisation. We hope that the reduction in contact between the metal and the vessel wall will lead to better rates of post-procedure subarachnoid haemorrhage in our patients.”
In July 2017 the US Food and Drug Administration (FDA) issued a notice announcing that Penumbra had recalled 150 3D revascularisation devices in the USA. The notice stated: “Penumbra is recalling the Penumbra 3D revascularisation device because there is a risk of the delivery wire breaking or separating during use. Fractured pieces of the delivery wire could be left inside the patient’s brain bloodstream, and this, or the attempts made to retrieve the fractured pieces, can make the stroke worse. This can also cause other serious adverse health consequences such as continued blockage of blood vessels, completion of the stroke, and death. On 9 June, 2017, Penumbra sent an Urgent Voluntary Removal notice to all affected customers. The notice asked customers to identify and remove any affected 3D revascularisation devices from inventory and quarantine.”
Following his SNIS presentation, Delgado clarified that all of the affected devices have now been returned to Penumbra and the device is safe for use.










