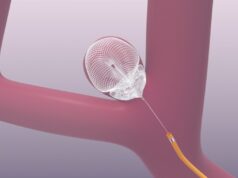
New technology in the form of a magnetically-assisted remote-controlled catheter (MARC) which could allow physicians to see and assess brain tissue more clearly while treating a stroke may hold promise, according to study authors who released their findings at the Society of NeuroInterventional Surgery (SNIS) 11th Annual Meeting in Colorado Springs, USA.
The findings stand to advance the field of neurointervention. Neurointerventionists typically accomplish this approach by manually directing the catheter and visualising its progress under standard X-ray guidance.
With MARC, study authors sought to understand if a remote-controlled catheter under Magnetic Resonance Imaging (MRI) guidance could more effectively accomplish manoeuvring through complex vessel anatomy, which would ultimately allow improved visualisation of the brain tissue affected during a stroke. “Given that MRI is the gold standard by which we determine brain tissue viability, it is exciting that we potentially now have new MRI-compatible technology that enables us, while treating a stroke, to make real-time assessments about whether brain tissue is dead or alive,” says Steven Hetts, lead study author and associate professor of Radiology at the University of California, San Francisco, USA. “The implications are numerous, including improved medical decision-making, which would naturally result in optimising patient safety and clinical outcomes.”
To assess the performance of MARC, Hetts and his colleagues aimed to determine mean procedure times and success data for a custom, clinical-grade MARC prototype under MRI guidance as compared to a manually-navigated catheter, under both MRI and conventional x-ray guidance – each procedure utilising a cryogel vascular model designed to simulate the main and branch blood vessels in a living human. The MRI-guided procedures were performed at 1.5T (magnetic field strength of a standard clinical MRI scanner) using a balanced steady-state free precession sequence in the type of clinical MRI scanner available in most hospitals.
Results showed that MARC was clearly visible under MRI guidance and was used to successfully complete 192 (80%) of 240 total turns around blood vessels as compared to the manually- directed catheter under both MRI and x-ray guidance, at 144 (60%) of 240 total turns and 119 (74%) of 160 total turns, respectively. MARC also was faster than the manually directed catheter under MRI, with a mean procedure time of 37 seconds per turn as compared to 55 seconds, but comparable to the manually directed catheter under X-ray guidance which required a mean of 44 seconds for each turn. When assessing the time required to navigate the various angles of branch vessels at turns of 45°, 60°, and 75°, MARC proved to be faster than the manually-directed catheter under MRI guidance.
“Given that the success of neurointerventional stroke treatment is directly tied to how fast and accurately physicians can eliminate the impact of a clot and restore blood flow to viable portions of the brain, technology that facilitates this objective stands to be transformative,” says Hetts. “By proving that MRI-guided neurointervention could be more effective than current standard approaches to stroke treatment, we are taking a significant step forward in the advancement of our field.”