CERENOVUS have announced the first patients have been treated with its new EMBOTRAP II Revascularisation Device since it became commercially available in the US. EMBOTRAP II is a next generation stent retriever used to capture and remove life-threatening blood clots from the brain following an ischaemic stroke. The company received US Food and Drug Administration (FDA) clearance to market the mechanical clot removal, or thrombectomy, device in May and is launching EMBOTRAP II at this week’s Society of NeuroInterventional Surgery (SNIS) 15th Annual Meeting.
“The EMBOTRAP II is an important new device for treating stroke patients and an important advancement in mechanical thrombectomy,” said Andrew DeNardo, an interventional neuroradiologist with Goodman Campbell Brain & Spine, who along with John Scott, Daniel Sahlein, and Richard Paulsen, recently performed thrombectomies with the device at Indiana University Health Methodist Hospital and St. Vincent Hospital in Indianapolis, USA.
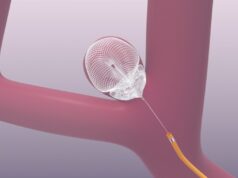
The EMBOTRAP II Device, with its proprietary dual-layer design, engages and grips stroke-inducing blood clots differently than other stent retrievers, allowing a doctor to maintain engagement and control of the clot with minimal compression during removal. It is indicated for use within eight hours of symptom onset.
“Blood clots can originate in different parts of the body, resulting in different clot types,” said Scott. “These different clot types present unique retrieval challenges during mechanical thrombectomy. The design of the EMBOTRAP II Device helps minimise these challenges and my early experience has been positive.”
In the ARISE II (Analysis of Revascularisation in Ischaemic Stroke with EMBOTRAP device) study published earlier this year in the journal, Stroke, neurointerventional stroke physicians restored blood flow in 80% of patients treated within three passes and in about half of patients within a single pass. At the 90-day follow-up, more than two-thirds were functionally independent. The study included 228 patients with large vessel occlusions and moderate to severe neurological deficits.