The identification of patients likely to benefit from stroke clot removal may be made more accurate with the use of brain imaging, rather than relying on the amount of time since symptoms began , according to research presented at the American Stroke Association’s International Stroke Conference (ISC 2016).
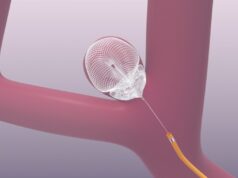
Evaluating data on 102 patients who have had endovascular therapy up to 18 hours after the start of their stroke, and had a computed tomography (CT) perfusion imaging scan before treatment, showed where a large area of brain tissue may be safely salvaged.
Good recovery—defined as little to no disability—was achieved in 71.4% of the patients treated within six hours and 61.7% of patients treated beyond six hours of stroke onset. There was no significant association between time to treatment and good outcomes when CT perfusion imaging showed salvageable brain tissue.
“Using this image-based selection, we would be able to look at any patient who comes through the door to identify the ones likely to benefit from these therapies, regardless of what the clock shows,” says Jenny Tsai, study author and neuroimaging and vascular neurology fellow at the Stanford Stroke Center, Palo Alto, USA. The facility is part of the University of Stanford’s School of Medicine.
“This is important because we want to offer the best treatments to every patient who suffers stroke and who may benefit from them. One of the best ways to do this is to have an objective imaging tool to evaluate every single patient,” she says.
Researchers analysed patient data from the clinical study CT Perfusion to Predict Response to Recanalisation in Ischemic Stroke Project (CRISP). The two-year study focused on adults 18 and older and finished in 2014. It was funded by the NIH and conducted at six US medical sites with the goal of developing a practical tool to identify acute stroke patients likely to benefit from endovascular therapy.
“We now have a very effective treatment for the large and disabling acute strokes,” Tsai says. “And we know that there are patients likely to benefit from interventional treatments who are not being captured using basic imaging and time criteria alone. We need to do better.”