
Following the recent introduction of key data supporting the use of high-frequency spinal cord stimulation (SCS) in the treatment of non-surgical refractory back pain (NSRBP), Leonardo Kapural (Carolinas Pain Institute, Winston-Salem, USA) details what these findings mean for a patient population that, up to now, has been largely undertreated.
Acute back pain causes more disability around the world than any other condition1 and a quarter of US adults report they have experienced back pain within the past three months.2 NSRBP is particularly troubling, with more than 500,000 patients experiencing pain but few widespread treatment options.3 Beginning in the 1990s, efforts to improve pain management resulted in a four-fold increase in the rate of opioid prescribing, disregarding the addictiveness, low therapeutic ratio, and lack of documented effectiveness of opioids in the treatment of chronic pain.4 While a recent study by the American Medical Association (AMA) showed the prescription rate of opioids has declined over the last 10 years, the country is now facing a worsening drug-related overdose and death epidemic.
This highlights several related things. The number of patients living with chronic pain has not decreased, leading to the assumption that patients who have come to depend on opioids for their pain management are now turning to less-controlled medical and non-medical pain management. Prioritising the outcomes, research and access to evidence-based pain management options is a viewpoint echoed by both the American Academy of Neurology and the AMA.
An example of this is the well-documented use of SCS to treat chronic pain. When CMM is not working, SCS should be considered. Of the 500,000 patients experiencing NSRBP, fewer than 5% have been offered SCS treatment.5 There are various SCS options on the market for various conditions, but multiple studies point to the efficacy of high-frequency SCS. In contrast to low-frequency (40–60Hz) SCS, high-frequency (10kHz) SCS is paraesthesia-independent and uniquely provides direct neural inhibition to the dorsal horn.
I recently presented 12-month outcomes from the SENZA-NSRBP randomised controlled trial (RCT) at the 25th North American Neuromodulation Society (NANS) annual meeting (13–15 January 2022; Orlando, USA), which documented the efficacy of high-frequency 10kHz therapy in subjects with NSRBP. One of the main drivers for this study was to collect validation for a specific NSRBP indication and coverage expansion—given that many eligible patients have access limitations due to commercial insurance barriers. The study, which supported the US Food and Drug Administration (FDA) approval of expanded labelling for the high-frequency Senza system (Nevro), has since been published in the Journal of Neurosurgery: Spine. Senza is now the only SCS system with specific labelling to treat NSRBP patients.
The SENZA-NSRBP RCT was designed to specifically study SCS therapy in the NSRBP population. Some 159 patients confirmed by neurosurgeon evaluation as non-surgical candidates and who failed medical management were randomised 1:1, undergoing CMM with and without utilisation of 10kHz SCS. The back pain responder rates were significant, with 78.2% of the 10kHz therapy subjects achieving ≥50% pain relief at 12 months. The average pain relief (percentage reduction of visual analogue scale [VAS] score from baseline) was 72.1%. In the crossover arm, 78.2% of participants reported pain relief of >50%, and the average pain relief was 70.4%, after using 10kHz therapy for six months.
Furthermore, a profound relief (>80%) was achieved in 50% of the subjects using 10kHz SCS therapy. We also concluded that 10kHz SCS reduces and, at times, eliminates opioid requirements in NSRBP patients. Fifty percent of subjects reduced their daily opioid dose by half, and 28% eliminated opioid use completely. These data indicate that high-frequency SCS should be used as part of the NSRBP treatment algorithm.
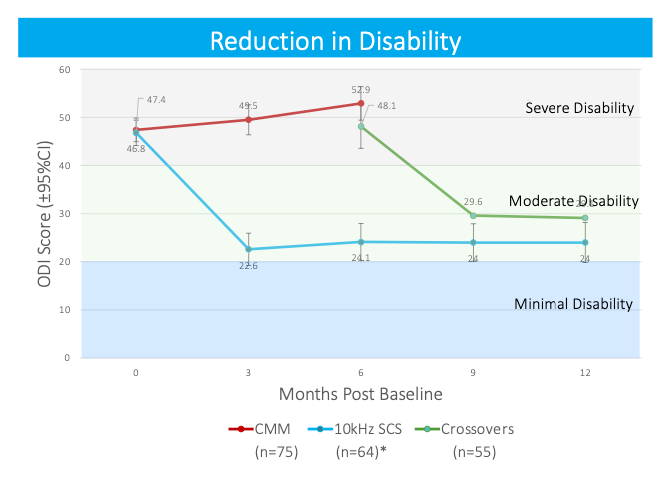
This study provided key insight into the durability of high-frequency SCS therapy for these patients. We saw long-term improvements in pain level, opioid use and overall quality of life. We also saw effective and sustained improvements in functional capacity, with 75% of subjects experiencing a more than 10-point Oswestry Disability Index (ODI) score reduction. Both initial 10kHz and crossover study groups’ reductions in disability remained stable through 12 months.
The data analysed in SENZA-NSRBP add to the growing body of clinical evidence of high-frequency SCS, and not only speaks to the durability of the pain relief and quality of life measures at 12 months but also provides the data input necessary for payers to expand coverage to this undertreated patient population. In conclusion, these study data support high-frequency SCS in NSRBP patient populations, and additional studies validate its use in chronic back and leg pain6, and painful diabetic neuropathy.7
References:
- Hoy D, March L, Brooks P et al. The Global Burden of Low Back Pain: Estimates from the Global Burden of Disease 2010 Study. Ann Rheum Dis. 2014; 73(6): 968–74.
- Deyo R A, Mirza S K, Martin B I. Back Pain Prevalence and Visit Rates: Estimates from U.S. National Surveys, 2002. Spine (Phila Pa 1976). 2006; 31(23): 2724–7.
- Sources: US Census Bureau; CLBP Market Research; CMS OP Hospital SAF Data 2012–2018. www.neuromodulation.com/failed-back-surgery-syndrome-definition.
- Frieden T R, Houry D. Reducing the Risks of Relief—the CDC Opioid Prescribing Guideline. NEJM. 2016; 374: 1501–4.
- Kapural L, Jameson J, Johnson C et al. Treatment of nonsurgical refractory back pain with high-frequency spinal cord stimulation at 10 kHz: 12-month results of a pragmatic, multicenter, randomized controlled trial. Journal of Neurosurgery: Spine. 2022. DOI: 10.3171/2021.12.SPINE211301.
- Kapural L, Yu C, Doust M W et al. Comparison of 10-kHz High-Frequency and Traditional Low-Frequency Spinal Cord Stimulation for the Treatment of Chronic Back and Leg Pain: 24-month Results from a Multicenter, Randomized, Controlled Pivotal Trial. Neurosurgery. 2016; 79(5): 667–77.
- Petersen E A, Stauss T G, Scowcroft J A et al. Durability of High-Frequency 10-kHz Spinal Cord Stimulation for Patients With Painful Diabetic Neuropathy Refractory to Conventional Treatments: 12-Month Results From a Randomized Controlled Trial. Diabetes Care. 2022; 45(1): e3–e6.
Leonardo Kapural is a partner and pain physician at the Carolinas Pain Institute in Winston-Salem, USA, and the Center for Clinical Research and BestOpinionDoctor.com. His interests include peripheral nerve stimulation, spinal cord stimulation, discogenic low back pain and visceral abdominal pain. He served as professor of anaesthesiology at the Cleveland Clinic Lerner College of Medicine of Case Western University (Cleveland, USA) and Wake Forest University (Winston-Salem, USA).
DISCLOSURES: Kapural is a consultant to Biotronik, Medtronic, Nalu, Presidio and Saluda Medical, and leads clinical research with Biotronik, Gimer Medical, Medtronic, NeuraLace, Neuros Medical, Nevro and Saluda.







