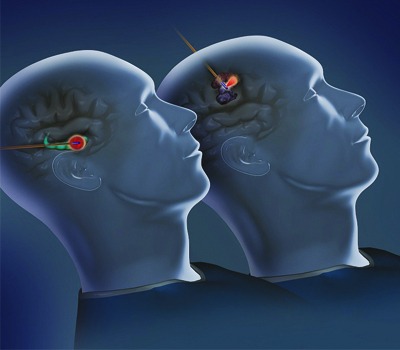
Monteris Medical has announced recent data demonstrating that newly diagnosed brain tumour patients undergoing procedures with the NeuroBlate system, a minimally invasive robotic laser thermotherapy tool, experienced improved outcomes. These findings, along with a separate case study presentation highlighting the first successful ablation of the hippocampus and amygdala using a directional laser, were presented during the 2015 Congress of Neurological Surgeons Annual Scientific Meeting (26–30 September, New Orleans, USA).
“To date, limited data have been available on brain tumour patients that received magnetic resonance imaging-guided laser ablation,” said Alireza Mohammadi, a neurosurgeon from Ohio. “This multicentre study, which also included cases from Washington University in Saint Louis and Yale-New Haven Hospital, is the largest series of laser ablation for patients with newly diagnosed glioblastoma lesions ever conducted and shows that NeuroBlate has an impact on both overall and progression-free survival on patients after surgery. While additional prospective studies are warranted, these preliminary findings are encouraging.”
In the first study, a multicentre review, investigators collected data from 22 patients with newly diagnosed glioblastoma tumours who underwent a procedure with the NeuroBlate system and who had not received prior radiation or chemotherapy. Extent of ablation was defined by software as blue (43 degrees centigrade for 10 minutes) or yellow (43 degrees centigrade for two minutes) thermal-damage threshold (TDT)-lines. Volumetric analysis was performed to determine the extent-of-coverage (EOC) by TDT lines.
EOC for yellow and blue TDT-lines was 94% and 91% respectively. Median overall survival and progression-free survival were 14.7 (range 2.7-44.2) and 5.4 months (range 3.4-9.2) respectively. Regression analysis for overall survival was significant for EOC by yellow and blue TDT-lines (p=0.04 for each), age (p=0.02) and pre-operative Karnofsky Performance Status or KPS (p=0.04). Additional analysis demonstrated that EOC by blue TDT-line was still significant for overall survival when compared with age (p=0.007) and had a good trend (p=0.08) versus KPS. Of note, EOC by yellow TDT-line was the only significant factor for progression-free survival (0.047).
Also, as part of the CNS scientific program, investigators from Vanderbilt University presented a case study highlighting their first successful ablation of the hippocampus and amygdala using the NeuroBlate SideFire directional laser.
Commenting on the case, Joseph Neimat, study author and associate professor of neurological surgery noted, “While brain structures with regular shapes can be readily targeted with laser therapy, complex structures have historically posed a challenge with this modality. A directional laser enabled contouring in the hippocampus and amygdala, regions that would otherwise be difficult to ablate. These findings, while preliminary, help lay the foundation for maximally precise, minimally-invasive lesioning of targets in the brain including tumours, seizure foci and low-flow vascular lesions.”
“We are encouraged by the growing body of scientific evidence supporting the use of NeuroBlate as a minimally invasive tool to ablate brain lesions,” said John Schellhorn, president and chief executive officer of Monteris Medical. “We are grateful to our clinical collaborators for advancing these studies and presenting their findings at this important scientific forum.”