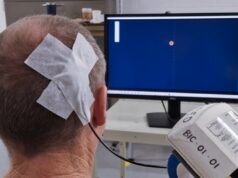
The third Stroke Recovery and Rehabilitation Roundtable—an initiative of the International Stroke Recovery and Rehabilitation Alliance (ISRRA)—has made a series of key recommendations about managing fatigue, measuring mobility, harnessing non-invasive brain stimulation technologies, and improving how trials are designed, recently publishing its advice in a special edition of the International Journal of Stroke.
The third Stroke Recovery and Rehabilitation Roundtable—an initiative of the International Stroke Recovery and Rehabilitation Alliance (ISRRA)—has made a series of key recommendations about managing fatigue, measuring mobility, harnessing non-invasive brain stimulation technologies, and improving how trials are designed, recently publishing its advice in a special edition of the International Journal of Stroke.
Kate Hayward (University of Melbourne, Melbourne, Australia) co-chaired and convened the current roundtable, which was initially established by Julie Bernhardt—a fellow stroke expert from the Florey Institute of Neuroscience and Mental Health—in 2016.
“The roundtables aim to address gaps that are hampering progress across the field of stroke recovery and rehabilitation,” said Hayward. “Momentum is gathering in stroke recovery and it is so important that we work together, pulling in the right direction, for the benefit of the millions of people globally who are affected by stroke.
“Post-stroke fatigue, for instance, is common and complex, yet very little is known about it. To address this, an expert panel of researchers and people living with stroke sought to define fatigue, create a roadmap for future research and design a new fatigue assessment tool.”
“The vision of our International Stroke Recovery and Rehabilitation Alliance is a world where global collaboration leads to major breakthroughs for people with stroke,” Bernhardt added. “Consensus building with these international taskforce recommendations is having impact and are an essential part of us achieving our vision.”
Fatigue after stroke
The fatigue panel, led by Coralie English (University of Newcastle, Callaghan, Australia) and Gillian Mead (University of Edinburgh, Edinburgh, UK), noted that fatigue affects almost half of all people living with stroke, yet there are no clear recommendations for preventing, recognising, treating or managing it.
The taskforce defined post-stroke fatigue as “a feeling of exhaustion, weariness or lack of energy that can be overwhelming, and which can involve physical, emotional, cognitive and perceptual contributors, which is not relieved by rest and affects a person’s daily life”.
They recommended that everyone who has had a stroke be assessed using a new Stroke Fatigue Clinical Assessment Tool, which asks a series of questions to ensure that fatigue is not missed, and to draw attention to potentially modifiable factors. The panel further recommended future research investigates psycho-education interventions, such as cognitive behavioural therapy, exercise, anti-depressants and neuromodulation therapies.
“For many people living with stroke, fatigue is their number one issue,” said English. “For too long, this area of stroke recovery has been neglected in research. We hope our paper will inspire researchers to work in this area and motivate breakthroughs that will improve the lives of people living with post-stroke fatigue.”
Non-invasive brain stimulation
A second panel, led by Jodi Edwards (University of Ottawa, Ottawa, Canada) and Numa Dancause (University of Montreal, Montreal, Canada), focused on finding ways to eliminate barriers for the use of non-invasive brain stimulation technologies as a treatment for stroke rehabilitation.
The expert panel found that there is experimental and clinical evidence supporting such technologies as safe and potentially effective adjuncts to therapy post-stroke, yet their use is largely limited to treating major depression and pain.
“Our panel sought to identify missing evidence for how to optimise these technologies for use as a standard treatment in post-stroke care,” said Edwards. “Surprisingly, we found that, in addition to evidence gaps, there were major limitations with existing trials. This means as a field we are much farther from having the evidence necessary to optimise these technologies than initially thought. We propose a set of core recommendations, and put forward a new checklist for future studies and clinical trials to help advance the field of brain stimulation post-stroke towards a pathway for translation to the clinic.”
Mobility and stroke
A third panel, led by Gert Kwakkel (Amsterdam University Medical Center, Amsterdam, The Netherlands) and Geert Verheyden (KU Leuven, Leuven, Belgium), recommended ways researchers can improve data on post-stroke mobility—a key priority for stroke survivors.
The mobility panel said it was essential for researchers to use standardised instruments to enable data from different projects to be compared. The members also agreed on metrics, definitions and instruments that researchers should use to measure aspects of mobility including balance, walking independence and walking endurance.
“Mobility problems are experienced by 80% of stroke survivors and often the most important goal for many post-stroke as it affects their independence, and quality of life,” said Kwakkel. “However, mobility is a complex construct that encompasses different domains that require different measurement instruments to assess recovery. In this panel, we achieved consensus on how and when to measure balance and mobility problems of people included in stroke recovery and rehabilitation studies.”
Research trials
The fourth roundtable, led by Hayward as well as Catherine Lang (Washington University, St Louis, USA), focused on trial design, and more specifically the control comparator group used in preclinical and clinical trials of stroke recovery interventions.
This panel developed the Control Design (CONSIGN) decision support tool to address challenges identified and enhance control comparator selection, description, and reporting.
“Identifying an appropriate type of control to use in a preclinical or clinical trial is challenging, yet critically important,” Hayward added. “The benefit of an experimental intervention is established relative to a prespecified control, and poor selection can reduce the ability to demonstrate a difference between the two.”