Advertorial
Health services across Europe have now implemented new policies to sustain the development of thrombectomy procedures. England’s National Health Service (NHS England) has made a commitment to expand availability of thrombectomy through specialised commissioning with a target of up to 8,000 procedures in the coming years.
Leading the way in this expansion is St George’s Hospital, London, UK, which has the first fully staffed 24/7 thrombectomy service in the country and the highest number of thrombectomy procedures performed in England. The organisation of regional stroke networks, patient care pathways, hospital stroke teams, as well as the use of imaging for both triage and endovascular guidance, have all played a major role in the growth of thrombectomy services.
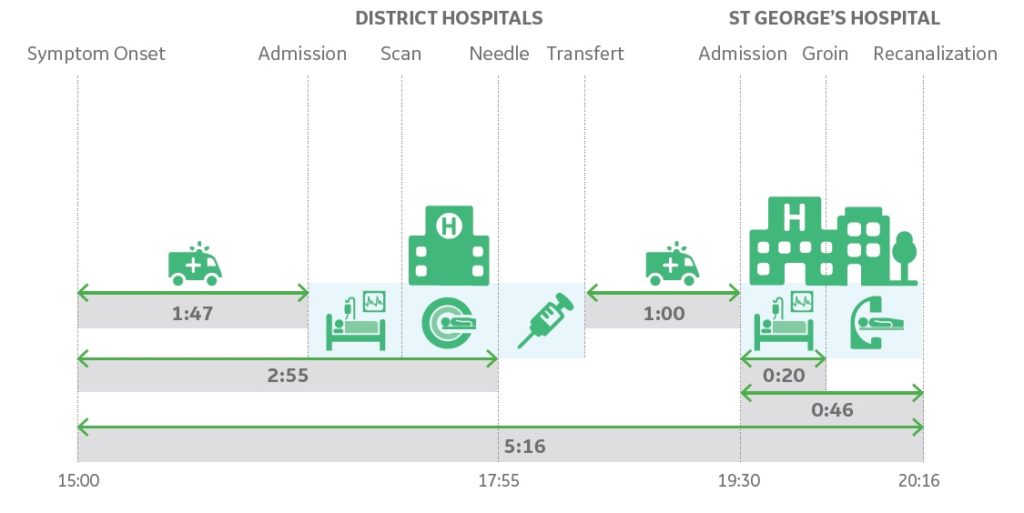
A consultant interventional neuroradiologist at St George’s Hospital, Jeremy Madigan, explained that the centre operates a hub and spoke model: St George’s (hub) accepts patients from its pre-defined catchment area. One of the biggest challenges with this model is ensuring the prompt repatriation of these patients. He says that access to the right advanced imaging, particularly CT angiography (CTA), in the referral centres is still a challenge in some places. This is being improved with teaching sessions to raise awareness of the importance of CTA within district hospitals.
Madigan said that the introduction of the 24/7 service was gradual, where they slowly introduced the daytime working hours at the weekend and then extended to longer days (8am to 8pm). The staff increased from three neurointerventionalists to five, and from five nurses to 10. The department also increased the number of radiographers and neuroanaesthetists. Before switching to 24/7, the team worked to make sure they had ironed out most of the problems. The idea was to ensure that they had robust procedures of how to deal with problems that may arise during working hours so that there would be no difficulty out of hours.
A key step was to create a separate entrance to the hospital for ambulances that are coming from the district hospital so that they do not have to go via the emergency department or the main entrance. They can arrive at a dedicated door and pick up the telephone and say that they have arrived. There are two entrances to the hospital for stroke patients: one to the accident and emergency department (A&E) for direct admissions and one to the neuroscience department, including diagnostic and interventional neuroradiology, for referred patients.
 As for the imaging protocols that have been implemented as part of the updated stroke policies, Madigan referred to the use of CT perfusion imaging, which he said gives a lot more confidence to the decision of moving forward with the thrombectomy. At St George’s Hospital the stroke team is now performing perfusion on all the patients whether they are presenting there or coming from a remote hospital. Part of the reason for this is that a portion of the patients that are received in good time and treated quickly with effective recanalisation still experience outcomes consistent with a big stroke.
As for the imaging protocols that have been implemented as part of the updated stroke policies, Madigan referred to the use of CT perfusion imaging, which he said gives a lot more confidence to the decision of moving forward with the thrombectomy. At St George’s Hospital the stroke team is now performing perfusion on all the patients whether they are presenting there or coming from a remote hospital. Part of the reason for this is that a portion of the patients that are received in good time and treated quickly with effective recanalisation still experience outcomes consistent with a big stroke.
“We assume that a stroke may be occurring between the time that they are referred from an outside hospital to the time we receive them. By performing the perfusion imaging on arrival we feel more confident that we are still doing the right thing by proceeding with the thrombectomy. We have had several cases recently where we received patients who developed a large established infarct and we opted not to proceed with the thrombectomy. If we are in the middle of a procedure and are concerned about a potential vessel rupture, we use Innova CT HD (available on GE biplane IGS 630) cone-beam CT. It is very good at showing sub-arachnoid haemorrhage of a decent volume and deep parenchymal haemorrhage as well,” Madigan said.
He added that the stroke thrombectomy service will continue to evolve, especially in response to new data that are being released expanding the criteria for thrombectomy treatment.
This advertorial has been sponsored by GE Healthcare