This advertorial is sponsored by Philips.
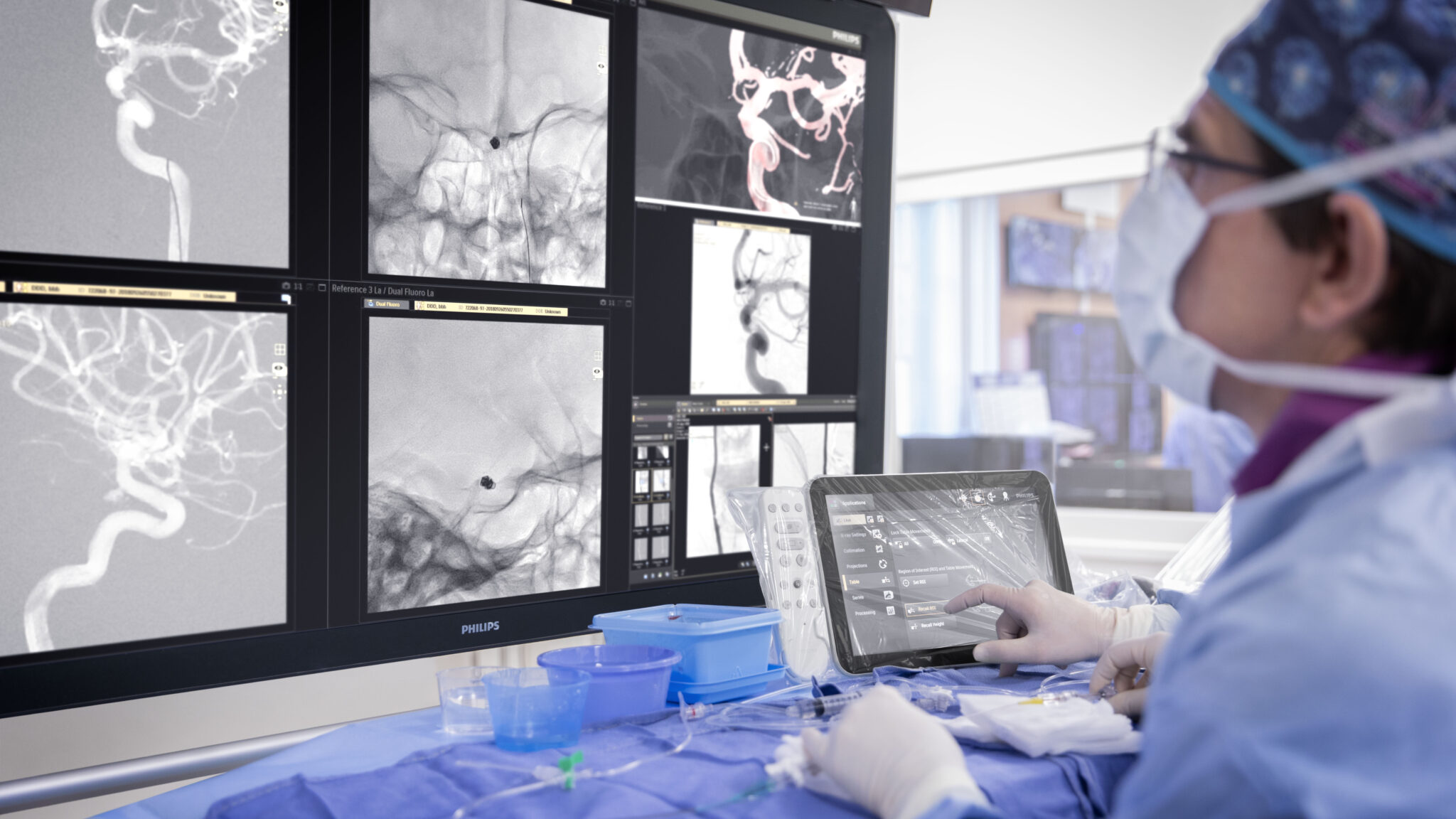
Time is of the essence when treating a patient who has just experienced a stroke. Every minute counts, and minimising the number of minutes a stroke is left untreated could be the difference for a person to recover or experience lasting disabilities.
Globally, one in four adults over the age of 25 will suffer a stroke in their lifetime.1 Healthcare teams understand every minute is crucial to saving a stroke victim’s life, yet gaps persist between communication, information and access to stroke experts. Stroke is a leading cause of disability, and the second leading cause of death worldwide2, so how can healthcare teams work faster and communicate more efficiently?
Today, physicians have access to a range of time-saving tools to support decision-making and treatment. As a leader in stroke care, Philips offers a diverse portfolio of stroke care solutions, including advanced technology for monitoring and communication in ambulances; telestroke patient assessment; diagnostic imaging and analysis; image-guided therapy; remote monitoring, and more.
While these end-to-end stroke care solutions, along with Direct to Angio Suite (DTAS) workflow and artificial intelligence (AI), are helping reduce time to treatment today, a re-examination of treatment guidelines may also lead to dramatic improvements in patient care. This is particularly important for patients who experience stroke symptoms upon waking up in the morning, called ‘wake-up patients’, which account for roughly one in five acute ischaemic strokes.

“Current stroke guidelines should be reviewed and updated based on findings from recent studies,” says Wim van Zwam, interventional radiologist at Maastricht University Medical Center in Maastricht, The Netherlands. “Patients in the early window should not receive advanced imaging to prevent unnecessary treatment delay and this is how we should consider wake-up patients. For some of these patients, time is very limited and we have to work quickly for them to benefit from revascularisation treatment.”
Reimagining standard practice stroke guidelines
Guidelines are meant to be followed; however, this does not mean it should not be improved upon, if possible. This is exactly what ‘challenging the status quo’ means and what patients expect from healthcare professionals in order to receive better care.
Van Zwam’s study, the MR CLEAN-LATE trial, which was presented at the recent World Stroke Congress (WSC 2022; 26–29 October, Singapore), enrolled many wake-up stroke patients who were all considered—according to current guidelines—as ‘late-onset’ stroke patients.3,4 However, evidence is building that the vast majority of wake-up stroke patients had their stroke onset shortly before waking up.4 This suggests that wake-up stroke patients should not be treated as late-onset strokes but rather as early-window patients, counting time from the moment they woke up.
By treating these patients as early-window strokes, wasted time due to advanced imaging work can be avoided and they can be provided a medicine called tissue plasminogen activator (tPA), which is only recommended in the first 4.5 hours. Patients can then be taken directly to angio in case of a large vessel occlusion (LVO). This new guideline revolutionises how stroke patients are taken care of and improves their outcome.
A one-stop stroke shop: DTAS
“The Direct to Angio Suite workflow provides valuable, time-saving support for transfer and direct patients who arrive at the comprehensive stroke center (CSC),” says Marc Ribó interventional neurologist at University Hospital Vall d’Hebron in Barcelona, Spain. “The goal is to treat patients faster while improving clinical outcomes.”
Currently, when a person experiences a stroke, emergency medical services are called upon to make two choices: go to the nearest hospital or go a little bit further to a specialised clinic for treatment. It is critical to get this decision right to avoid wasting time, yet wasted time is all too common. For example, in a study of 7,000 patients, 40% of the time from symptom onset to treatment occurred within the hospital walls.5
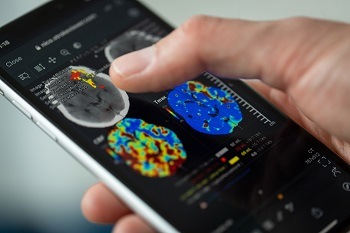
To reduce this time, Philips partnered with Nicolab to bring a cloud-based, end-to-end, AI-based stroke triage and management solution— StrokeViewer—that aims to improve patient outcome by optimising the stroke workflow. StrokeViewer analyses computed tomography (CT) scan data with AI, and automatically detects LVO and its location. StrokeViewer then shares this analysis with physicians at both primary stroke centres (general radiologists and neurologists) and intervention centres (stroke neurologists, interventional neurologists and radiologists) where the patient is eventually treated.
“With AI, teams at the stroke center can decide which hospital to refer the patient, where to take them so they can go straight to thrombectomy,” states Rotem Sivan-Hoffman, head of the Radiology Department at Meir Medical Center in Haifa, Israel, and founder and chief medical officer at CVAid. “The promise of AI means patients have the opportunity for early detection, precise diagnosis and personalised treatment.”
AI’s role in stroke care optimisation
For stroke care teams to work rapidly, act decisively and deliver the best stroke patient outcomes, information, technologies and people across the stroke care pathway must be connected. AI-based decision support tools can help do this across the entire continuum of stroke care, from informing emergency medical services of the patient’s stroke status, to prehospital and hospital stages, to radiology.
“Philips is dedicated in working to detect strokes faster and supporting communication between care teams so they can make accurate, quick decisions to get patients treated as fast as possible,” says Angelique Balguid, head of Marketing for Neurovascular Portfolio at Philips. “Bridging the gaps that slow down doctors is about connecting the dots across the entire patient journey and, with the help of AI integration, we can improve patient outcomes.”
Improving the patient experience
By refining the decision-making process, and increasing access to technology and expertise, stroke patients can have a better chance of receiving adequate treatment in time.
Continuing to improve upon the ‘standard’ care for stroke patients is imperative to overcome current challenges hospitals are facing. Embracing technology and including this into the design of the stroke care pathway may help to manage the patient load, and have better patient selection, yet provide better care. With the rising demand for improved stroke care, an increase in AI application will support keeping pace while delivering better quality standard of care to patients for generations to come.
Rotem Sivan-Hoffman, Wim van Zwam and Marc Ribó discussed reimagining stroke care during a webcasted industry session at this year’s. You can watch their discussion here.
References:
1. https://www.world-stroke.org/world-stroke-day-campaign/why-stroke-matters/learn-about-stroke.
2. Katan, M; Luft, A. Global Burden of Stroke. Semin Neurol. 2018; 38(2): 208–11.
3. Pirson, A F A V; Hinsenveld, W H; Goldhoorn, R J B et al. MR CLEAN-LATE, a multicenter randomized clinical trial of endovascular treatment of acute ischemic stroke in The Netherlands for late arrivals: study protocol for a randomized controlled trial. Trials. 2021; 22(1): 160.
4. Cheng, B; Pinnschmidt, H; Königsberg, A et al. Estimating nocturnal stroke onset times by magnetic resonance imaging in the WAKE-UP trial. Int J Stroke. 2022; 17(3): 323–30.
5. Silver, B; Arnold, M. Implications of the WAKE-UP Trial. Stroke. 2018; 49(12): 3115–7.











