
As middle meningeal artery embolisation (MMAe) for chronic subdural haematoma (cSDH)—already bolstered by randomised trial data and, more recently, by multiple US Food and Drug Administration (FDA) device approvals—continues to gain traction, its real-world utility will inevitably be placed under the microscope. Here, neurointerventionists Jan Gralla (Bern, Switzerland) and Gowtham Kuncha (Madurai, India) outline the integral role that flow model-based simulations could play in ensuring operators can safely attain the necessary experience and skillsets required to administer these treatments as a part of routine clinical practice.
CSDH is among the most frequent neurosurgical diagnoses in elderly patients, with recurrence after surgical evacuation posing a persistent challenge. In recent years, MMAe has progressed from an experimental adjunct to an evidence-based interventional therapy. Randomised controlled trials have demonstrated that MMAe significantly reduces recurrence and reoperation rates, firmly establishing its role within modern cSDH treatment algorithms.
The strength of MMAe lies in its pathophysiological approach. Rather than addressing only the mass effect of the haematoma, embolisation targets the vascularised neo-membranes responsible for ongoing inflammation and microhaemorrhage. This shift has positioned endovascular therapy as a disease-modifying intervention. As a result, neurointerventionists now play a central role in the multidisciplinary management of this disease, with a growing responsibility in procedural execution and long-term outcomes.
Material selection and technical considerations
Several embolic materials are currently used for MMAe, each with distinct characteristics. Particulate agents, such as polyvinyl alcohol (PVA) particles, were adopted early due to their simplicity and availability. However, their tendency toward proximal occlusion limits distal penetration and raises concerns about durable devascularisation.
Liquid embolics have therefore gained prominence. Several randomised trials have demonstrated the clinical benefit of non-adhesive ethylene-vinyl alcohol (EVOH)-based agents that enable controlled, fluoroscopically guided distal embolisation. Cyanoacrylate glues, including newer formulations with slower polymerisation, offer immediate and permanent occlusion without the need for dimethyl sulfoxide (DMSO), but demand advanced technical expertise due to their adhesive nature and narrower safety margin.
Despite its minimally invasive nature, MMAe carries risks. Understanding the anatomy of the external carotid artery and potentially dangerous anastomoses—especially with the ophthalmic circulation, petrosal branches, and cranial nerve supply—is crucial. Non-target embolisation, reflux-related complications and cranial neuropathies, though rare, emphasise the importance of meticulous super-selective catheterisation and controlled embolic injection techniques. As distal penetration improves with liquid agents, technical errors become more likely, underscoring the need for structured operator training and careful case selection.
Scaling uptake while consolidating experience
As MMAe adoption expands across centres, procedural dissemination is progressing while cumulative operator experience is still consolidating. With the rapid expansion of MMAe, structured training for young interventional physicians has become a clinical necessity. In high-volume centres, procedural confidence develops through repeated exposure and mentorship. However, as the technique disseminates to centres with varying case volumes, structured preparation becomes increasingly important. Although the MMAe procedure may seem technically straightforward, subtle differences in vascular anatomy, flow dynamics and embolic behaviour can have major consequences. Therefore, operator experience remains a key determinant of safety and efficacy, particularly when using liquid embolics or glues.
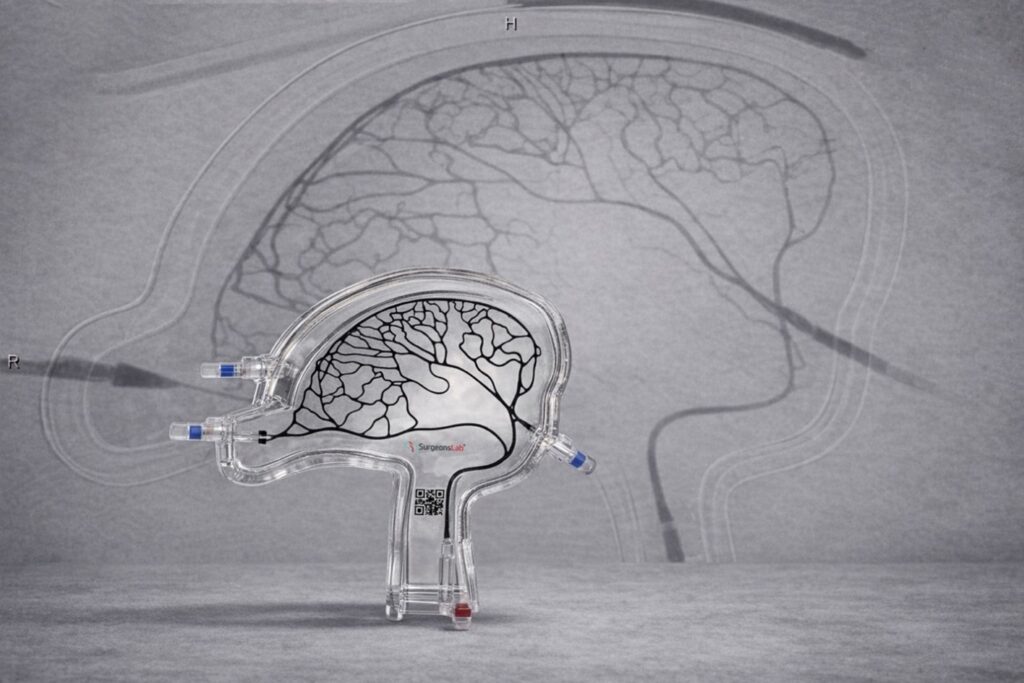
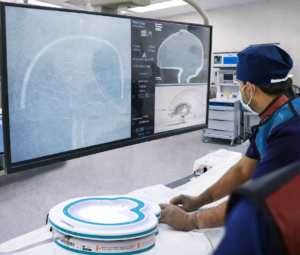
In this context, simulation-based learning and in-vitro flow models are emerging and gaining importance as complementary educational tools in neurointerventional training. Flow models that replicate the MMA and its distal branches allow operators to rehearse distal navigation, understand catheter stability, and study injection dynamics, reflux behaviour and embolic penetration patterns of different materials in a controlled environment. Hands-on sessions using dedicated MMA flow models that simulate various vessel calibres, retrograde flow configurations and neo-membranes provide practical insights and training prior to clinical application. Such structured training may help reduce variability during early operator experience, and serve as a bridge between theoretical knowledge and live procedural practice.
Embolising with liquid agents in flow models can provide operators with a practical understanding of how navigation in small vessels works; how differing embolic agents behave under flow and injection rate; and how distal penetration and proximal preservation vary. This can be repeated multiple times within the same model on a reusable MMAe simulator. There is significant scope to improve training—particularly for junior colleagues who need firsthand experience before approaching complex cases.
Training as a cornerstone of responsible adoption
Although simulation cannot be a substitute for real-world mentorship or clinical judgment, it enables trainees to learn from errors in a controlled environment rather than on patients. Simulation is instrumental in understanding the nuanced behaviour of EVOH-based agents and cyanoacrylate glues, thereby reducing the learning curve and enhancing procedural confidence. These models provide a safe platform for skill acquisition, material comparison and procedural standardisation before clinical application. Flow-based, reusable MMAe training simulators exemplify integration of procedural rehearsals into workshops and structured training programmes.
As indications for MMAe increase and techniques advance, the future success of this emerging treatment will depend not only on material innovation but also on high-quality training and simulation-based education that prepare the next generation of interventionists to provide safe, durable and effective care.
The authors declared no relevant disclosures.
Jan Gralla is the head and director of the Institute of Diagnostic and Interventional Neuroradiology at the Inselspital of the University Hospital of Bern in Bern, Switzerland. He is also the current chair of the Internal Affairs Committee for the European Society of Minimally Invasive Neurological Therapy (ESMINT).
Gowtham Kuncha is a consultant microvascular and endovascular neurosurgeon at the Meenakshi Super Speciality Hospital in Madurai, India.









