
Recent evidence demonstrating the effectiveness of endovascular treatment with mechanical thrombectomy for acute ischaemic stroke due to proximal large vessel occlusion in the anterior circulation, and its superiority over standard therapy including intravenous thrombolysis, has completely changed the approach to this disease in the acute setting. As mechanical thrombectomy has become the standard of care for these patients, health providers must face new challenges for its implementation. First, it is mandatory to make it available and to ensure equality of access for all eligible patients. Second, the process to correctly diagnose, select patients and provide treatment, should be fast enough to achieve success.
Considering the complexity and expense ofendovascular procedures, effectively organised systems of care are necessary for an efficient implementation within the community, which is of particular relevance for public health systems that must deal with budget issues. Networking between all the differentstages in the care chain for health provision is essential for this purpose. The Madrid Stroke Network is a good example of a collaborative system of care at a regional level, aimed to provide the optimal specialised treatment for any patient suffering from an acute ischaemic stroke, including prompt access to a stroke unit facility, to IV thrombolysis and to endovascular procedures if necessary.
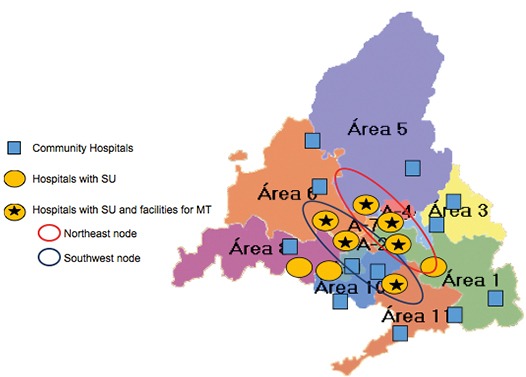
The Autonomous Community of Madrid is a region of Spain with a population of around 6.5 million inhabitants. The metropolitan area of the city of Madrid is surrounded by a rural area, the longest distance from the centre being 100 km. Madrid has a public Health System comprising of 15 community hospitals and nine hospitals with stroke units that have a neurologist available 24h/7d. Six of the hospitals with stroke units are equipped with all the resources and technical support to perform mechanical thrombectomy. Each hospital has its own catchment area, but the network has been organised to ensure rapid transfer of patients with the suspicion of an acute stroke directly to the nearest hospital with a stroke unit for prompt, specific treatment (ie. intravenous thrombolysis), thus avoiding delays due to initial attention in small community hospital not equipped with the necessary resources. Secondary transfers from the community hospital to the stroke unit are also possible if necessary, and specialised support by a neurologist via telestroke systems has been implemented between one of the stroke units and one community hospital in order to be able to initiate treatment as soon as possible with ulterior transfer to the stroke unit (drip-and-ship paradigm). Once in a stroke unit, protocols for rapid diagnosis—including neurovascular imaging—and treatment of patients are applied. For provision of endovascular treatment 24h/7d in the whole area of Madrid, six of the qualified hospitals have been organised in two collaborative nodes (Northeast and Southwest), consisting of three hospitals each, that are grouped based on proximity and catchment area, one of which is on-call in a weekly rotating shift. Thus, everyday there are two centres in Madrid capable of providing mechanical thrombectomy for suitable patients, each one covering half the geographic area and the population of the region.
 Every patient meeting criteria is transferred to the corresponding on-duty hospital for mechanical thrombectomy from the first-attending stroke unit after initial evaluation and treatment. Occasionally, patients can be transferred directly to the on-duty hospital for mechanical thrombectomy based on clinical data from the forewarning made by the emergency medical systems, provided agreement between the stroke unit and the hospital on-duty for mechanical thrombectomy. After treatment, once the patient is stable they are transferred back to the referral stroke unit, thus avoiding overload of the treating hospital during the period that it is on-call.
Every patient meeting criteria is transferred to the corresponding on-duty hospital for mechanical thrombectomy from the first-attending stroke unit after initial evaluation and treatment. Occasionally, patients can be transferred directly to the on-duty hospital for mechanical thrombectomy based on clinical data from the forewarning made by the emergency medical systems, provided agreement between the stroke unit and the hospital on-duty for mechanical thrombectomy. After treatment, once the patient is stable they are transferred back to the referral stroke unit, thus avoiding overload of the treating hospital during the period that it is on-call.
This collaborative networking permits the sharing of resources and costs thus making implementation of mechanical thrombectomy in the clinical routine affordable (shared-care model). The system has demonstrated not only efficiency, but also efficacy, since it has extended the treatment opportunity to a greater number of candidate patients with results regarding procedural times, recanalisation rates, and outcomes that are similar to those from clinical trials and that are continuously improving.
Some key factors have been essential for accomplishing this achievement. First, a close collaboration between stroke neurologists and the public health authorities to make an adequate plan based on estimation of needs for an adjusted setting up of resources. Second, involvement of all professionals that participate in acute stroke care, including emergency services, community hospitals, hospitals with stroke units, and referral hospitals for mechanical thrombectomy, in elaboration of and compliance with protocols for diagnosis, treatment and transfer of patients, that ensure a rapid and efficient workflow. Third, registration of all cases, procedures, outcomes and complications in a shared database is crucial for continuous monitoring of performance that helps to identify pitfalls and failures and to enable continuous improvement of the process.
Actually, monitoring of our performance has allowed us to identify some opportunities of improvement, mainly to reduce onset-to-treatment times and futile secondary transfers. One important issue is repetition of diagnostic tests, mainly neuroimaging, when a patient is transferred for mechanical thrombectomy. Rapid transmission of clinical data and neurovascular imaging, as well as a fluent communication between the treating physicians are crucial to avoid repetition of tests that could be unnecessary and that may add unacceptable delays in initiation of treatment. Also, we have verified that one of the major sources of delay in treatment is the time taken in secondary transfers. This is really difficult to reduce even in an organised network in which collaborating hospitals are quite close one from the other. Routing patients directly to the hospital on call for mechanical thrombectomy would result in shorter times to treatment at the cost of an overload of the emergency room with patients that might not be eligible once evaluated. Accurate selection of patients that are very likely to be suitable for mechanical thrombectomy by the emergency services would be desirable, and efforts should be made to develop reliable tools that could be used for pre-hospital patient selection.
In summary, the Madrid Stroke Network experience could serve as an example for development of collaborative networks for provision of endovascular treatment in other cities. The particular characteristics of the area should be taken into account to ensure feasibility and efficacy.
References
1 Alonso de Leciñana M, Fuentes B, Ximénez-Carrillo A, et al. A collaborative system for endovascular treatment of acute ischaemic stroke: the Madrid Stroke Network experience. Eur J Neurol 2016; 23: 297–303.
2 Fuentes B, Alonso de Leciñana M, Ximénez-Carrillo A, et al. Futile interhospital transfer for endovascular treatment in acute ischemic stroke. Stroke 2015; 46: 2156–61.
María Alonso de Leciñana, Blanca Fuentes, and Exuperio Díez-Tejedor are at the Department of Neurology and Stroke Centre, University Hospital La Paz, Autónoma University of Madrid, Spain













